Spider veins, also known as thread veins, are a cluster of small, superficial, damaged blood vessels. They are visible under the skin and resemble cobwebs…
Can Spider Veins On Legs Be Invisible? What To Know
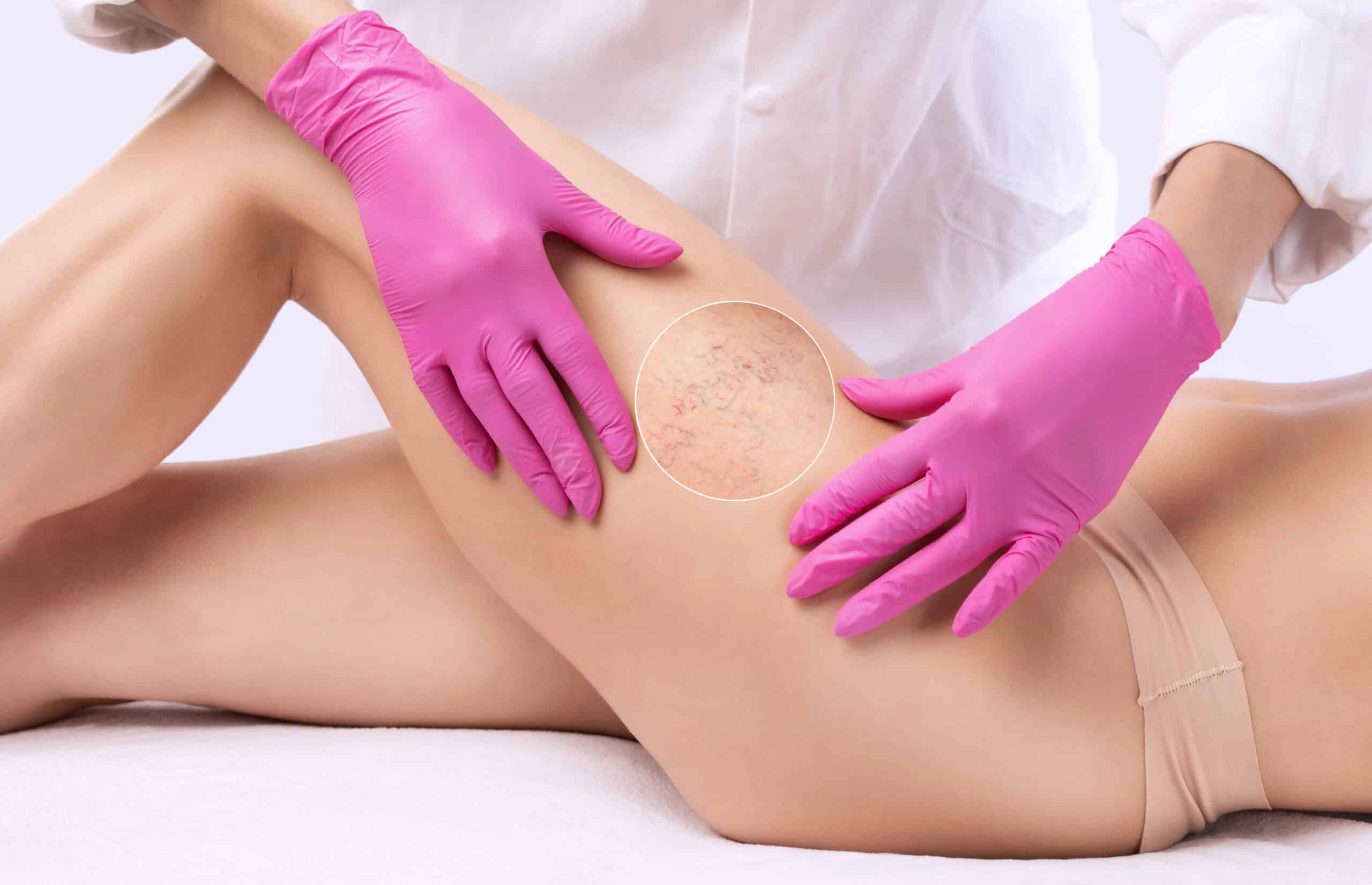
Spider veins, also known as thread veins, are a cluster of small, superficial, damaged blood vessels. They are visible under the skin and resemble cobwebs or tree roots, with thin, curvy lines that branch out from a central point. They may be red or blueish-purple in color, but spider veins deeper under the skin won’t always be visible.1
Spider veins are generally harmless and do not cause any pain. They are usually found on the face and legs. Most people don’t experience any serious medical symptoms associated with spider veins, so treatments for this condition are geared toward cosmetic improvements.2
What Are the Symptoms of Spider Veins?
Spider vein is a colloquial term for telangiectasia. Unlike varicose veins, which are thick, ropelike veins, spider veins are thin and thread-like.3
Spider veins usually occur due to abnormalities in the network of capillaries in the skin. Venous spider veins are usually between 1 millimeter and 3 millimeters in diameter.4 In the legs, they are only around 180 micrometers to 1 millimeter deep under the skin.5
Varicose veins can be associated with uncomfortable symptoms like pain, swelling, and itching. Conversely, spider veins are relatively asymptomatic. Because they are small and superficial, they may be visible under the skin, but spider veins don’t bulge like varicose veins.6
In some cases, symptoms like burning, itching, pain, heaviness, or tiredness of the legs may occur. Occasionally, cramping and throbbing have also been reported with special circumstances such as standing or walking for long hours or during menstruation.7
Can Spider Veins Be Invisible?
Invisible spider veins refer to spider veins that are developing due to exposure to various risk factors. Hidden spider veins usually involve a deeper venous network and may not be visible on the surface.
The term “hidden varicose veins” was introduced in 2011 to refer to underlying veins that reflux, even if the bulging veins aren’t visible on the surface. However, in such cases, the underlying causes and mechanism of disease are expected to be the same as visible varicose veins.8
Varicosities in larger veins cause blood pooling, resulting in increased pressure. This pressure pushes the excess blood into smaller veins or capillaries, causing spider veins.9
Similarly, invisible or hidden varicose veins may lead to the development of hidden spider veins on legs.
The exact cause of spider veins remains unknown. However, increased blood pressure in the lower limbs can cause spider veins. In the face, spider veins are more likely to occur due to sun exposure or injury.10
The likelihood of having spider veins increases with age as exposure to risk factors also increases. Some of the risk factors that can promote the development of spider veins include:11
- Age: Spider veins have been reported in 41% of women older than 50 years.12 This is because your veins are more likely to weaken and become damaged with age.
- Hormonal changes: The sex hormone estrogen relaxes blood vessel walls, increasing your chance of developing spider veins. Conditions such as menstruation, pregnancy, or menopause and hormone treatments like birth control pills can be risk factors for spider veins.
- Heredity: Spider veins are more likely to occur in people whose family members also exhibit this condition.
- Weight changes: Spider veins can be caused by excess body weight, which can lead to increased blood pressure on your legs. Conversely, sudden or dramatic weight loss could reveal previously hidden spider veins.
- Lifestyle: Prolonged sitting or standing in the same position can cause spider veins by increasing the blood pressure in your legs.
- Injury and exposure: Injuries and sunburns can be risk factors for spider veins. The sun’s harmful rays can damage the vein walls and form spider veins.
What Are Signs To Watch Out For?
Spider veins occurring due to increased body weight or hormonal changes may be temporary and could resolve on their own.13
However, the symptoms of spider veins could also worsen with time if no treatment is provided, particularly in cases where the deeper veins have been affected. Blood clots can develop at such sites.14
So, if you notice any of the abovementioned symptoms like pain, burning, itching, throbbing, or discomfort, consider seeking treatment even if no spider veins are visible.
What Are the Treatments for Spider Veins?
Spider vein treatments are usually aimed at providing aesthetic benefits. Spider veins typically resolve within three to six weeks of treatment and are unlikely to recur.15
Treatment can include lifestyle changes such as a healthy diet, regular exercise, avoiding prolonged sun exposure without sunscreen, sitting or standing for long periods, and restrictive clothing. Treatments that provide symptomatic relief include leg elevation and gradient compression stockings to improve blood circulation.
Although spider veins don’t require as much treatment as varicose veins, minimally invasive procedures are available for spider vein treatment.
Sclerotherapy (injection therapy)
The sclerotherapy technique involves a minimally invasive, brief procedure. It’s simple, relatively painless, and can be completed within an hour.16
This technique injects a chemical called a sclerosant into the problematic vein. Once it enters the vein, this sclerosant begins to irritate the vein walls. This causes the vein to collapse and become sealed. The blood is rerouted into the healthy veins, and the body gradually reabsorbs the sealed vein.
Due to its minimally-invasive nature, you can recover quickly and easily after sclerotherapy. Your daily activities are unlikely to be impacted by treatment.17
Laser treatment
Laser therapy is a noninvasive procedure for treating tiny spider veins that occur just below the skin’s surface. This technique applies a powerful laser beam to the area containing the spider veins. Damaged veins are sealed and dried out by laser energy. This allows blood to flow through the surrounding healthier veins, easing the pressure.
Although some skin darkening or discoloration may occur in the treated area due to the laser treatment, this is only temporary and will resolve in a few months.18
Ohmic thermolysis
Ohmic thermolysis is also known as radiofrequency thermocoagulation (VeinGogh or ThermaVein). This is an efficient and advanced technique for curing spider veins. High-frequency microbursts of targeted heat energy are delivered into the damaged vein (spider vein) using a machine with a needle. The vein walls collapse and are closed up by the heat energy. The blood flow diverts to the healthy veins, and the damaged spider veins are gradually reabsorbed.19
This procedure is also used to improve the success rate of other procedures such as sclerotherapy.20
Even after receiving treatment, continue to visit a vein specialist for regular follow-ups to prevent a recurrence.
Look for a Vein Specialist
Although relatively harmless, the presence of multiple spider veins on your face or legs can make you feel self-conscious about your appearance. But spider vein treatment is now really simple and just a step away.
If you’re unsure how to get started, My Vein Treatment’s vein specialist locator tool can assist you in finding a suitable vein specialist near you, so you don’t have to travel far for treatment. Book an appointment today to receive the best treatment guidance and be free of displeasing spider veins.
SOURCES:
- OASH: “ Varicose veins and spider veins.”
- Cochrane Database of Systematic Reviews: “ Treatment for telangiectasias and reticular veins.”
- OASH: “ Varicose veins and spider veins.”
- Journal of vascular nursing: official publication of the Society for Peripheral Vascular Nursing: “ Sclerotherapy of telangiectasias or spider veins in the lower limb: A review.”
- The Journal of dermatologic surgery and oncology: “ Do telangiectases communicate with the deep venous system?”
- Cochrane Database of Systematic Reviews: “ Treatment for telangiectasias and reticular veins.”
- Cochrane Database of Systematic Reviews: “ Treatment for telangiectasias and reticular veins.”
- Clinical, cosmetic and investigational dermatology: “ Current Best Practice in the Management of Varicose Veins.”
- American Academy of Dermatology: “ Leg Veins: Why They Appear and How Dermatologists Treat Them.”
- American Academy of Dermatology: “ Leg Veins: Why They Appear and How Dermatologists Treat Them.”
- OASH: “ Varicose veins and spider veins.”
- Cochrane Database of Systematic Reviews: “ Treatment for telangiectasias and reticular veins.”
- Phlebology: “ Adjuvant radiofrequency thermocoagulation improves the outcome of liquid sclerotherapy in the treatment of spider veins of the leg: A pilot study.”
- OASH: “ Varicose veins and spider veins.”
- American Academy of Dermatology: “ Leg Veins: Why They Appear and How Dermatologists Treat Them.”
- American Academy of Dermatology: “ Leg Veins: Why They Appear and How Dermatologists Treat Them.”
- Better Health Channel: “ Varicose veins and spider veins.”
- Cleveland Clinic: “ Sclerotherapy.”
- American Academy of Dermatology: “ Leg Veins: Why They Appear and How Dermatologists Treat Them.”
- Cochrane Database of Systematic Reviews: “ Treatment for telangiectasias and reticular veins.”





Responses