If you’re pregnant and have noticed a new bulging or discoloration in your leg veins, you’re not alone. Research shows that as many as four in…
Your Guide to Varicose Veins During Pregnancy

If you’re pregnant and have noticed a new bulging or discoloration in your leg veins, you’re not alone. Research shows that as many as four in every 10 pregnant women experience varicose veins — that characteristic swelling and bulging of the veins in the legs.
The good news is that varicose veins usually aren’t dangerous to your health. When they develop during pregnancy, they usually go away shortly after birth. In the meantime, though, they can be uncomfortable and make you self-conscious.
Fortunately, there are steps you can take to ease the symptoms of varicose veins in pregnancy. This article will cover what you need to know, starting with why pregnancy makes you more likely to get varicose veins.
What Causes Varicose Veins in Pregnancy?
Varicose veins develop due to weak or damaged valves inside the vein, usually in the legs. As the vessel walls get weaker, blood begins to pool in the vein and sometimes flows backward away from the heart. This causes the vein to swell, taking on the distorted appearance that’s characteristic of varicose veins.
Varicose veins are more common in older adults, but pregnancy also increases a person’s risk of developing them. There are two primary reasons why.
Hormones and Baby Weight
When you’re pregnant, your body produces more of the hormone progesterone — which relaxes the walls of your veins. Meanwhile, the weight of your developing baby puts more pressure on your pelvic and leg veins, especially the large vein that carries blood from the feet back to the heart.
This combination of pressure and weakened vein walls makes you susceptible to varicose veins. You can develop varicose veins at any time during your pregnancy, but the risk goes up as your baby grows, simply because there’s more weight on your lower body.
Other Risk Factors
You may be more likely to develop varicose veins in pregnancy if you have other risk factors, such as:
- Age. If you’re an older expectant parent, your risk of varicose veins may be higher.
- Excess weight. Being overweight or obese adds to the pressure on your veins
- Extended sitting or standing. If your work requires you to stand or sit for long periods of time, you may be more likely to get varicose veins during pregnancy, especially if you can’t modify your job while pregnant.
- Family history. If your close family members have varicose veins or had them during pregnancy, you’re more likely to develop them.
- Hormone treatments. Some research shows that if you’ve taken hormone-based birth control, you may be at increased risk of developing varicose veins.
Symptoms of Varicose Veins
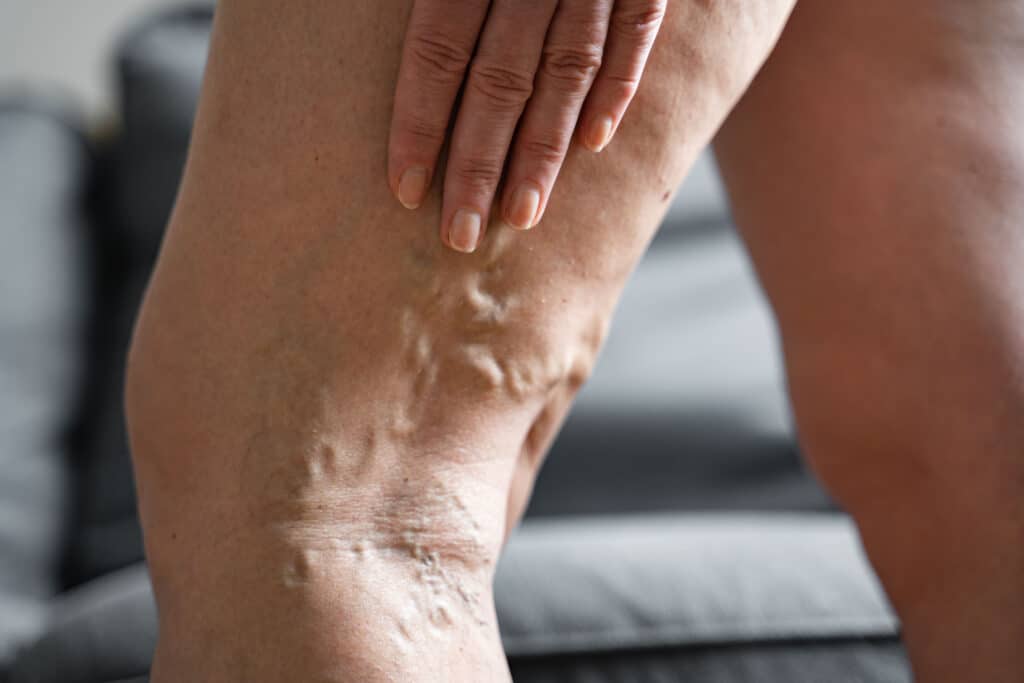
Many people see new varicose veins before they feel them. Varicose veins have a very distinct appearance — they look like bluish, twisted cords that bulge underneath the surface of the skin.
For some people, varicose veins are no more than a cosmetic annoyance. Others experience physical symptoms such as:
- Changes in skin color around the affected vein
- Dull, aching pain
- Feelings of heaviness or tenderness in the legs
- Leg cramps at night
- Swelling in the feet and ankles
These are only some of the symptoms associated with varicose veins. Because swollen leg veins can press on nearby nerves, some people also experience generalized pain and itching as well as other unusual sensations — like the feeling of water dripping down the leg or bugs crawling on the skin.
These sensations can be unnerving, but they’re normal and usually nothing to worry about. It’s also normal for your varicose veins symptoms to get worse when you sit or stand for a long time and improve when you lie down.
How to Prevent Varicose Veins
It’s not always possible to completely prevent varicose veins or get them to go away. The circulatory and hormonal changes of pregnancy are inevitable — as your baby grows, it naturally puts more strain on your legs.
That doesn’t mean that everyone who gets pregnant will develop varicose veins, but it does mean that you might not be able to avoid them.
Luckily, there are day-to-day lifestyle choices that you can make to keep your veins healthy and potentially help with your varicose vein symptoms. Consider adopting the following healthy habits:
- Avoid sitting or standing in the same position for a long time. Avoid sitting with crossed legs.
- Exercise regularly. If your doctor says it’s okay, daily low-impact exercise is best.
- Reduce your salt intake to keep vein inflammation down.
- Rest with your legs elevated above your heart.
- Sleep on your left side. This reduces pressure on the inferior vena cava, which is responsible for carrying blood back to the heart from your legs. When this vessel is healthy, your leg veins don’t have to work as hard.
- Take regular walking breaks throughout the day.
- Wear gradient compression stockings. These apply gentle pressure in the right spots to keep your blood flowing in the right direction.
Home remedies may not completely prevent or eliminate varicose veins for everyone, but they may reduce your symptoms and possibly help the veins to fade faster after birth.
When to Be Concerned
Varicose veins usually aren’t a cause for concern, but it’s always best to play it safe during pregnancy. Contact a vein specialist or your obstetrician if you experience any of the following symptoms:
- A broken or bleeding vein
- Flaky, discolored, fragile, or broken skin over your varicose veins
- Severe leg pain
- Varicose veins that are red, warm, or tender
If you’re concerned about your varicose veins for any reason, especially if they interfere with your daily life or don’t fade after you give birth, talk to a specialist.
My Vein Treatment’s vein specialist locator tool can help you to find someone in your area who can offer knowledgeable, compassionate advice and discuss potential treatments.





Responses