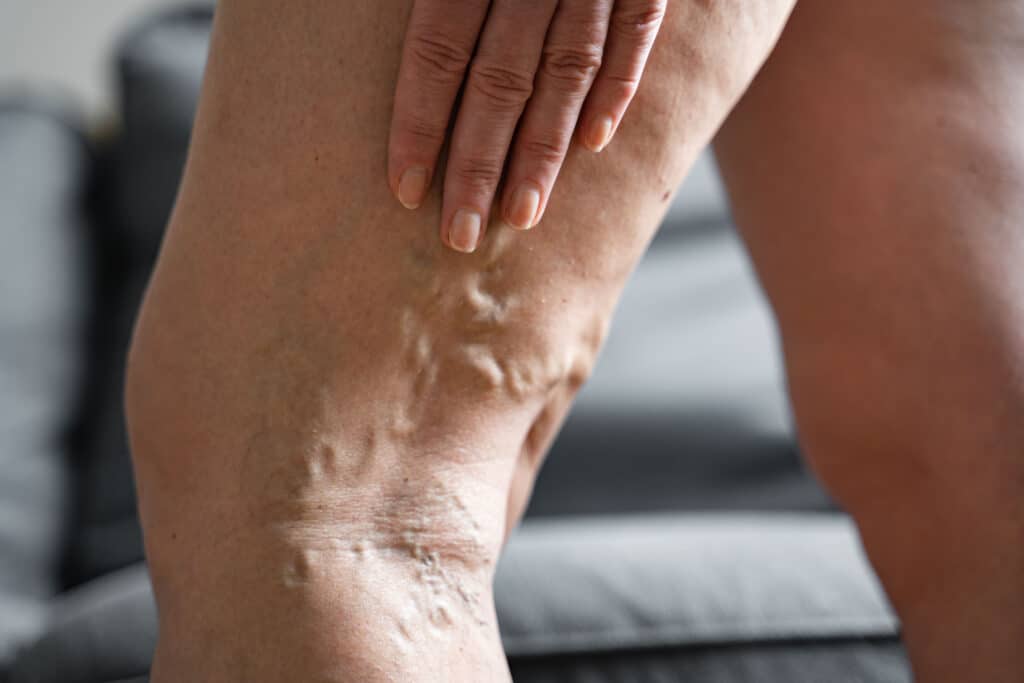
Millions of people struggle with the pain of varicose veins. Between 35% and 40% of Americans — more than a third — will develop varicose veins…
A Varicose Pain Treatment Quick Guide: 4 Noninvasive Solutions
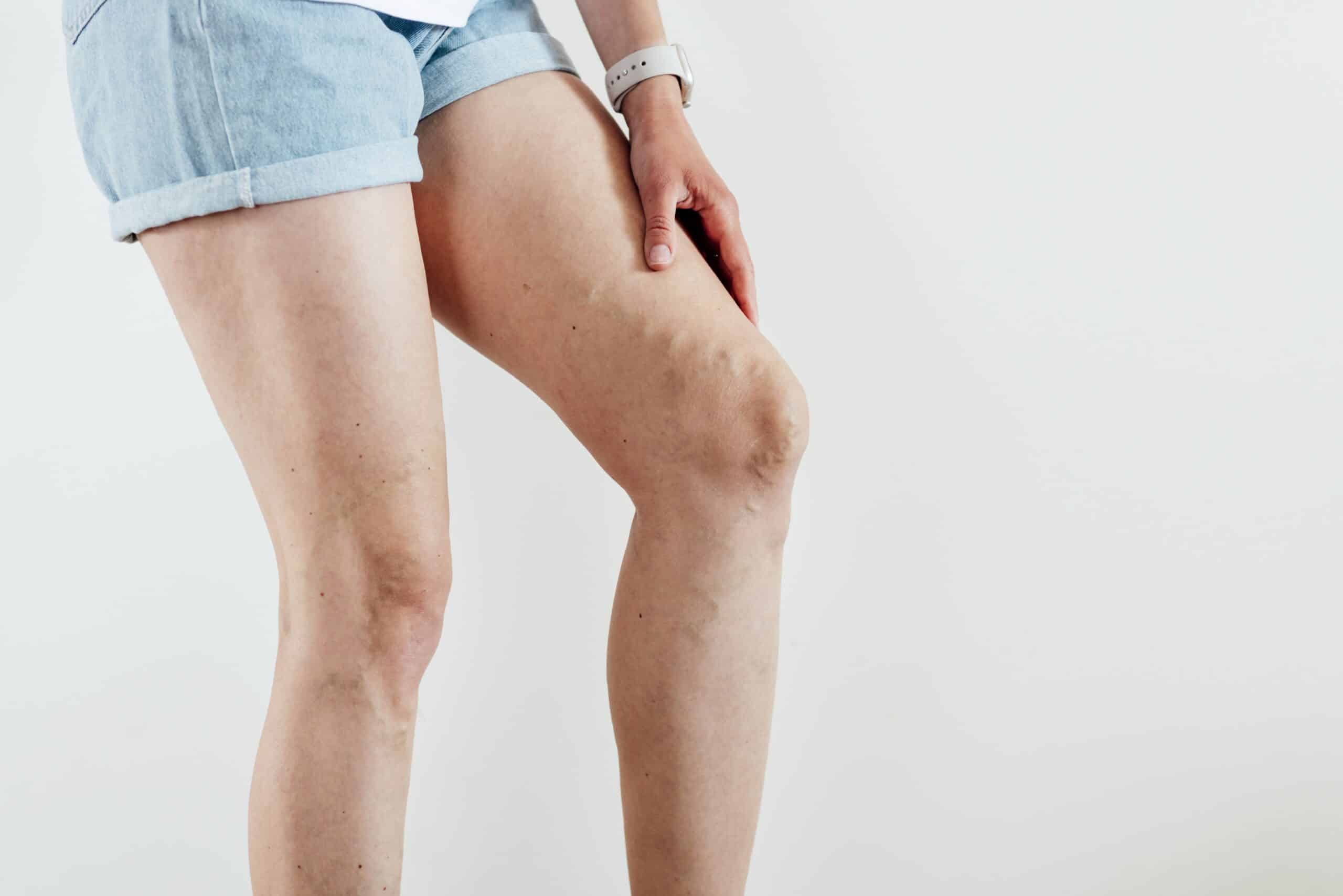
Millions of people struggle with the pain of varicose veins. Between 35% and 40% of Americans — more than a third — will develop varicose veins at some point during their lives. If you’re one of these millions, you may seek some varicose vein pain treatment.
Varicose veins are not usually dangerous but may cause uncomfortable symptoms like itching, throbbing, or heaviness in the legs. Experiences like these leave many patients wondering what causes varicose vein pain and if they need to see a doctor to get rid of it.
Varicose veins are typically caused by venous insufficiency, meaning that the veins have suffered damage and can’t effectively send blood back to the heart. Poor blood flow can cause blood to build up or flow in the wrong direction, causing pressure and further damaging the vein walls. As the veins stretch and bulge, they pressure the nearby nerves. The more pressure is involved, the worse the pain can get.
Fortunately, you can try several varicose vein treatment options at home. Here are four of the most effective.
1. Gradient Compression Stockings
Gradient compression stockings are special socks that support healthy circulation in the legs. They’re popular among distance runners, frequent fliers, and medical professionals who treat varicose veins and spider veins.
They work by encouraging blood to flow upward through the leg veins. Leg veins are among the hardest-working vessels in the circulatory system, constantly overcoming gravity to push blood toward the heart.
One-way valves help by closing behind the flow of blood. If those valves weaken or fail, blood can flow backward and pool in the veins. This stresses the valves and vein walls, potentially worsening varicose veins.
Gradient compression stockings are available in various sizes, colors, and price points. Quality will be an investment, but something that doesn’t work isn’t a bargain in the first place. When in doubt, ask a vein specialist for a recommendation.
2. Physical Activity
A sedentary lifestyle increases your risk of varicose veins and can worsen your symptoms. When you sit or stand for extended periods, your blood doesn’t flow as easily through your system. Your leg veins have to work harder, and blood is more likely to pool and press against the vein walls.
Keep your blood pumping by taking regular walking breaks throughout the day. Walking helps to activate your calf muscles and pushes the blood where it needs to go.1 The more your blood moves through the leg veins, the less strain you put on your varicose veins.
If you have a desk job, set reminders to get up and walk several times an hour. Wander down the hall and back or take the stairs to another floor. If you work from home, take a walk around the block.
Don’t like walking? Try dancing, biking, aerobic workouts, or any other exercise that keeps your legs moving. You can even do ankle circles or stretches at your desk.
3. Over-the-Counter Pain Medication
While varicose veins don’t cause physical discomfort for everyone, some people find the condition very painful. It may feel like burning, throbbing, or cramping in the affected area. The pain may be worse if you sit or stand for extended periods.
If you have varicose vein pain, over-the-counter medications like ibuprofen (Advil) or acetaminophen (Tylenol) may help. Ask your doctor if there are any medication types you need to avoid.
Always take over-the-counter medications according to the printed directions and safely dispose of expired medications.
4. Resting With Legs Elevated
Varicose veins often feel worse after resting because the blood has pooled in the legs. Rest with your legs elevated above your heart to reduce the risk of this happening.
Sleep with pillows or rolled blankets under your feet if possible. Put pillows on your couch or footstool so you can relax with your feet up. Leg elevation pillows are ideal. Elevating your legs lets gravity encourage the blood back to your heart, taking some of the load off your feet.
Limitations of Nonmedical Solutions
Lifestyle interventions like these can help relieve varicose veins symptoms. Some, including exercise and compression stockings, may slow the progression of varicose veins, so they don’t worsen as quickly. But none of the approaches above — or any other popular natural remedy — will fix existing damage to your veins.
To eliminate varicose veins or to get medical advice if your symptoms haven’t improved with home care, you need to visit a vein specialist. These medical professionals can evaluate your varicose veins and explain potential minimally invasive treatment options.
These options introduce an agent — heat or chemical — that seals the affected vein. When the vein closes, the body reroutes the blood through nearby healthy veins. Meanwhile, the treated vein dissolves, and the body eliminates it naturally. Examples:
- Endovenous laser ablation (EVLA) generates heat via laser energy
- Radiofrequency ablation (RFA) uses high-frequency radio energy
- VenaSeal uses a medical adhesive called cyanoacrylate
- Microfoam sclerotherapy uses a chemical foaming agent
All four options are safe and similarly effective. The recovery time is minimal, and many patients return to normal activities the same day. If this sounds appealing, your next step is to speak with a vein specialist.
Finding the Right Varicose Veins Pain Treatment
If you struggle to find a varicose veins pain treatment that works, a specialist can help. Varicose vein specialists offer proven treatments in comfortable and convenient office settings.
Learn more about available varicose vein treatments on My Vein Treatment, then use the specialist locator tool to find a specialist near you.
SOURCE:
1. The Journal of Venous Disease: ” Evaluation of physical activity level and exercise capacity in patients with varicose veins and chronic venous insufficiency.“